|
Overview
 A variety of foot problems can lead to adult acquired flatfoot deformity (AAFD), a condition that results in a fallen arch with the foot pointed outward. Most people - no matter what the cause of their flatfoot - can be helped with orthotics and braces. In patients who have tried orthotics and braces without any relief, surgery can be a very effective way to help with the pain and deformity. This article provides a brief overview of the problems that can result in AAFD. Further details regarding the most common conditions that cause an acquired flatfoot and their treatment options are provided in separate articles. Links to those articles are provided. Causes You can have a tendency towards fallen arches from birth. Up through the toddler stage, it is common to have flat feet. Throughout childhood, arches tend to normally develop. For reasons not well understood, however, in some cases the feet stay flat and the arch never forms. In many cases this abnormality does not cause symptoms or require any treatment. In other cases, it is due to a condition called tarsal coalition. This occurs when some of the foot bones fuse. Symptoms Pain and stiffness of the medial arch or anywhere along the mid-portion of the foot. Associated discomfort within and near the ankle joint. The knees, hips, and lower back may be the primary source of discomfort. Feet may often feel tired and achy. Painful shin splints may develop with activity. Gait may be awkward. Diagnosis Runners are often advised to get a gait analysis to determine what type of foot they have and so what kind of running shoe they require. This shouldn?t stop at runners. Anyone that plays sports could benefit from this assessment. Sports shoes such as football boots, astro trainers and squash trainers often have very poor arch support and so for the 60-80% of us who do overpronate or have flat feet they are left unsupported. A change of footwear or the insertion of arch support insoles or orthotics can make a massive difference to your risk of injury, to general aches and pains and even to your performance. Is flat footedness genetic? Non Surgical Treatment Custom orthotics are specially designed insoles, which are made for your by prescription. This is done by taking a plaster cast of the foot in its neutral position and is then sent to a laboratory, with your prescription to be made to your exact specifications. The insole then correctly aligns your foot and as a result your body. This will relieve abnormal strain of tissues and structures which can cause pain. For less severe mal-alignments or for sports use a wide variety of temporary insoles. Surgical Treatment  Surgical correction is dependent on the severity of symptoms and the stage of deformity. The goals of surgery are to create a more functional and stable foot. There are multiple procedures available to the surgeon and it may take several to correct a flatfoot deformity. Stage one deformities usually respond to conservative or non-surgical therapy such as anti-inflammatory medication, casting, functional orthotics or a foot ankle orthosis called a Richie Brace. If these modalities are unsuccessful surgery is warranted. Usually surgical treatment begins with removal of inflammatory tissue and repair of the posterior tibial tendon. A tendon transfer is performed if the posterior tibial muscle is weak or the tendon is badly damaged. The most commonly used tendon is the flexor digitorum longus tendon. This tendon flexes or moves the lesser toes downward. The flexor digitorum longus tendon is utilized due to its close proximity to the posterior tibial tendon and because there are minimal side effects with its loss. The remainder of the tendon is sutured to the flexor hallucis longus tendon that flexes the big toe so that little function is loss. Stage two deformities are less responsive to conservative therapies that can be effective in mild deformities. Bone procedures are necessary at this stage in order to recreate the arch and stabilize the foot. These procedures include isolated fusion procedures, bone grafts, and/or the repositioning of bones through cuts called osteotomies. The realigned bones are generally held in place with screws, pins, plates, or staples while the bone heals. A tendon transfer may or may not be utilized depending on the condition of the posterior tibial tendon. Stage three deformities are better treated with surgical correction, in healthy patients. Patients that are unable to tolerate surgery or the prolonged healing period are better served with either arch supports known as orthotics or bracing such as the Richie Brace. Surgical correction at this stage usually requires fusion procedures such as a triple or double arthrodesis. This involves fusing the two or three major bones in the back of the foot together with screws or pins. The most common joints fused together are the subtalar joint, talonavicular joint, and the calcaneocuboid joint. By fusing the bones together the surgeon is able to correct structural deformity and alleviate arthritic pain. Tendon transfer procedures are usually not beneficial at this stage. Stage four deformities are treated similarly but with the addition of fusing the ankle joint. Overview
While many people have slight differences in the length of one leg compared to the other, a significant difference between the two legs can cause problems. Leg length discrepancies can disturb the way a person walks, how his or her spine lines up and strain hip joints. Causes Some children are born with absence or underdeveloped bones in the lower limbs e.g., congenital hemimelia. Others have a condition called hemihypertrophy that causes one side of the body to grow faster than the other. Sometimes, increased blood flow to one limb (as in a hemangioma or blood vessel tumor) stimulates growth to the limb. In other cases, injury or infection involving the epiphyseal plate (growth plate) of the femur or tibia inhibits or stops altogether the growth of the bone. Fractures healing in an overlapped position, even if the epiphyseal plate is not involved, can also cause limb length discrepancy. Neuromuscular problems like polio can also cause profound discrepancies, but thankfully, uncommon. Lastly, Wilms? tumor of the kidney in a child can cause hypertrophy of the lower limb on the same side. It is therefore important in a young child with hemihypertrophy to have an abdominal ultrasound exam done to rule out Wilms? tumor. It is important to distinguish true leg length discrepancy from apparent leg length discrepancy. Apparent discrepancy is due to an instability of the hip, that allows the proximal femur to migrate proximally, or due to an adduction or abduction contracture of the hip that causes pelvic obliquity, so that one hip is higher than the other. When the patient stands, it gives the impression of leg length discrepancy, when the problem is actually in the hip. Symptoms Back pain along with pain in the foot, knee, leg and hip on one side of the body are the main complaints. There may also be limping or head bop down on the short side or uneven arm swinging. The knee bend, hip or shoulder may be down on one side, and there may be uneven wear to the soles of shoes (usually more on the longer side). Diagnosis There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference. Non Surgical Treatment Whether or not treatment should be pursued depends on the amount of discrepancy. In general, no treatment (other than a heel life, if desired) should be considered for discrepancies under two centimeters. If the discrepancy measures between two and five centimeters, one might consider a procedure to equalize leg length. Usually, this would involve closure of the growth plate on the long side, thereby allowing the short side to catch up; shortening the long leg; or possibly lengthening the short leg.  bestshoelifts Surgical Treatment Bone growth restriction (epiphysiodesis) The objective of this surgical procedure is to slow down growth in the longer leg. During surgery, doctors alter the growth plate of the bone in the longer leg by inserting a small plate or staples. This slows down growth, allowing the shorter leg to catch up over time. Your child may spend a night in the hospital after this procedure or go home the same day. Doctors may place a knee brace on the leg for a few days. It typically takes 2 to 3 months for the leg to heal completely. An alternative approach involves lengthening the shorter bone. We are more likely to recommend this approach if your child is on the short side of the height spectrum. Overview
 Heel pain is pain in the heel area that can vary in severity and location. It is most common in adults. The heel is the first bone to contact the ground when walking and takes the full force of impact and the resulting shock of bearing weight during motion. Causes Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation maybe aggravated by shoes that lack appropriate support and by the chronic irritation that sometimes accompanies an athletic lifestyle. Achilles Tendinopathy, Pain and inflammation of the tendon at the back of the heel that connects the calf muscle to the foot. Sever?s, Often found in children between the ages of 8 - 13 years and is an inflammation of the calcaneal epiphyseal plate (growth plate) in the back of the heel. Bursitis. An inflamed bursa is a small irritated sack of fluid at the back of the heel. Other types of heel pain include soft tissue growths, Haglunds deformity (bone enlargement at the back of the heel), bruises or stress fractures and possible nerve entrapment. Symptoms The symptoms of plantar fasciitis include pain along the inside edge of the heel near the arch of the foot. The pain is worse when weight is placed on the foot especially after a long period of rest or inactivity. This is usually most pronounced in the morning when the foot is first placed on the floor. This symptom called first-step pain is typical of plantar fasciitis. Prolonged standing can also increase the painful symptoms. It may feel better after activity but most patients report increased pain by the end of the day. Pressing on this part of the heel causes tenderness. Pulling the toes back toward the face can be very painful. Diagnosis After you have described your foot symptoms, your doctor will want to know more details about your pain, your medical history and lifestyle, including. Whether your pain is worse at specific times of the day or after specific activities. Any recent injury to the area. Your medical and orthopedic history, especially any history of diabetes, arthritis or injury to your foot or leg. Your age and occupation. Your recreational activities, including sports and exercise programs. The type of shoes you usually wear, how well they fit, and how frequently you buy a new pair. Your doctor will examine you, including. An evaluation of your gait. While you are barefoot, your doctor will ask you to stand still and to walk in order to evaluate how your foot moves as you walk. An examination of your feet. Your doctor may compare your feet for any differences between them. Then your doctor may examine your painful foot for signs of tenderness, swelling, discoloration, muscle weakness and decreased range of motion. A neurological examination. The nerves and muscles may be evaluated by checking strength, sensation and reflexes. In addition to examining you, your health care professional may want to examine your shoes. Signs of excessive wear in certain parts of a shoe can provide valuable clues to problems in the way you walk and poor bone alignment. Depending on the results of your physical examination, you may need foot X-rays or other diagnostic tests. Non Surgical Treatment Initial treatment should consist of an ice pack. Some runners prefer to use a wet towel that has been in the fridge. We recommend you use commercially available ice packs for focused pain released. An anti-inflammatory such as Ibuprofen will help to reduce the swelling. Please note this should be taken with meals and never before running. As with all soft tissue injuries, you may have to re-examine your training regime. A reduction or even a total break form running may be necessary. . Examine your running shoes, making sure the shoes do not bend excessively near the middle of the foot and at the ball of the foot. Sports shoes with built in insoles can be beneficial, however we recommend you replace existing insoles with specific sports orthotics/ insoles. Silicone heel cups, leather heel pads and contrasting cold and hot therapy can all help to speed up the healing process. The plantar fascia stretch will help to prevent the injury from occurring again. Please note that this stretch should not be done while the heel is inflamed and should only be attempted once you?re a feeling minimal or no pain from your heel. Surgical Treatment It is rare to need an operation for heel pain. It would only be offered if all simpler treatments have failed and, in particular, you are a reasonable weight for your height and the stresses on your heel cannot be improved by modifying your activities or footwear. The aim of an operation is to release part of the plantar fascia from the heel bone and reduce the tension in it. Many surgeons would also explore and free the small nerves on the inner side of your heel as these are sometimes trapped by bands of tight tissue. This sort of surgery can be done through a cut about 3cm long on the inner side of your heel. Recently there has been a lot of interest in doing the operation by keyhole surgery, but this has not yet been proven to be effective and safe. Most people who have an operation are better afterwards, but it can take months to get the benefit of the operation and the wound can take a while to heal fully. Tingling or numbness on the side of the heel may occur after operation. no foot pain Prevention  It may not be possible to prevent all cases of heel pain. However, there are some easy steps that you can take to avoid injury to the heel and prevent pain. Whenever possible, you should wear shoes that fit properly and support the foot, wear the right shoes for physical activity, stretch your muscles before exercising, pace yourself during physical activity, maintain a healthy diet, rest when you feel tired or when your muscles ache, maintain a healthy weight. Overview
Leg length discrepancy (LLD) affects about 70% of the general population, and can be either structural - when the difference occurs in bone structures - or functional, because of mechanical changes at the lower limbs. The discrepancy can be also classified by its magnitude into mild, intermediate, or severe. Mild LLD has been particularly associated with stress fracture, low back pain and osteoarthritis, and when the discrepancy occurs in subjects whose mechanical loads are increased by their professional, daily or recreational activities, these orthopaedic changes may appear early and severely. The aim of this study was to analyze and compare ground reaction force (GRF) during gait in runners with and without mild LLD. Results showed that subjects with mild LLD of 0.5 to 2.0 cm presented higher values of minimum vertical GRF (0.57 ? 0.07 BW) at the shorter limb compared to the longer limb (0.56 ? 0.08 BW) Therefore, subjects with mild LLD adopt compensatory mechanisms that cause additional overloads to the musculoskeletal system in order to promote a symmetrical gait pattern as showed by the values of absolute symmetric index of vertical and horizontal GRF variables.  Causes An anatomical short leg is due to several orthopedic or medical condition mechanisms. Often, one leg simply stops growing before the other one does and is called ?congenital?. We often see mother-daughters or father-sons who exhibit virtually the same degree of shortness on the same side. Often it is not known why this occurs, but it seems to account for approximately 25% of the population demonstrating a true LLD. Other causes of a true LLD include trauma or broken bones, surgical repair, joint replacement, radiation exposure, tumors or Legg-Calves-Perthes disease. Symptoms Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down. Diagnosis Leg length discrepancy may be diagnosed during infancy or later in childhood, depending on the cause. Conditions such as hemihypertrophy or hemiatrophy are often diagnosed following standard newborn or infant examinations by a pediatrician, or anatomical asymmetries may be noticed by a child's parents. For young children with hemihypertophy as the cause of their LLD, it is important that they receive an abdominal ultrasound of the kidneys to insure that Wilm's tumor, which can lead to hypertrophy in the leg on the same side, is not present. In older children, LLD is frequently first suspected due to the emergence of a progressive limp, warranting a referral to a pediatric orthopaedic surgeon. The standard workup for LLD is a thorough physical examination, including a series of measurements of the different portions of the lower extremities with the child in various positions, such as sitting and standing. The orthopaedic surgeon will observe the child while walking and performing other simple movements or tasks, such as stepping onto a block. In addition, a number of x-rays of the legs will be taken, so as to make a definitive diagnosis and to assist with identification of the possible etiology (cause) of LLD. Orthopaedic surgeons will compare x-rays of the two legs to the child's age, so as to assess his/her skeletal age and to obtain a baseline for the possibility of excessive growth rate as a cause. A growth chart, which compares leg length to skeletal age, is a simple but essential tool used over time to track the progress of the condition, both before and after treatment. Occasionally, a CT scan or MRI is required to further investigate suspected causes or to get more sophisticated radiological pictures of bone or soft tissue. Non Surgical Treatment You may be prescribed a heel lift, which will equal out your leg length and decrease stress on your low back and legs. If it?s your pelvis causing the leg length discrepancy, then your physical therapist could use your muscles to realign your pelvis and then strengthen your core/abdominal region to minimize the risk of such malalignment happening again. If you think that one leg may be longer than the other and it is causing you to have pain or you are just curious, then make an appointment with a physical therapist.  can gym help in increasing height? Surgical Treatment Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age. Overview
 Morton's neuroma is named after Dr Morton who first described this condition in 1876. It is sometimes called Morton's metatarsalgia or interdigital neuroma. It is a condition that affects one of the common plantar digital nerves that run between the long bones (metatarsals) in the foot. It most commonly affects the nerve between the third and fourth metatarsal bones, causing pain and numbness in the third and fourth toes. It can also affect the nerve between the second and third metatarsal bones, causing symptoms in the second and third toes. Morton's neuroma rarely affects the nerve between the first and second, or between the fourth and fifth, metatarsal bones. It tends to affect only one foot. It is rare to get two neuromas at the same time in the same foot. Morton's neuroma is named after Dr Morton who first described this condition in 1876. It is sometimes called Morton's metatarsalgia or interdigital neuroma. It is a condition that affects one of the common plantar digital nerves that run between the long bones (metatarsals) in the foot. It most commonly affects the nerve between the third and fourth metatarsal bones, causing pain and numbness in the third and fourth toes. It can also affect the nerve between the second and third metatarsal bones, causing symptoms in the second and third toes. Morton's neuroma rarely affects the nerve between the first and second, or between the fourth and fifth, metatarsal bones. It tends to affect only one foot. It is rare to get two neuromas at the same time in the same foot.Causes Morton's neuroma is an inflammation caused by a buildup of fibrous tissue on the outer coating of nerves. This fibrous buildup is a reaction to the irritation resulting from nearby bones and ligaments rubbing against the nerves. Irritation can be caused by Wearing shoes that are too tight. Wearing shoes that place the foot in an awkward position, such as high heels. A foot that is mechanically unstable. Repetitive trauma to the foot such as from sports activities like tennis, basketball, and running. Trauma to the foot caused by an injury such as a sprain or fracture. It is unusual for more than one Morton's neuroma to occur on one foot at the same time. It is rare for Morton's neuroma to occur on both feet at the same time. Symptoms Symptoms typically include pain, often with pins and needles on one side of a toe and the adjacent side of the next toe. Pain is made worse by forefoot weight bearing and can also be reproduced by squeezing the forefoot to further compress the nerve. Pressing in between the third and forth metatarsals for example with a pen can also trigger symptoms. Diagnosis You might first seek advice from your family doctor about your foot pain. He or she may refer you to a doctor or surgeon who specializes in foot disorders. Before your appointment, you may want to write a list of answers to the following questions. When did your symptoms begin? Did your symptoms begin gradually or suddenly? What type of footwear do you wear for work? Do you participate in sports? If so, what types in particular? What medications and supplements do you take regularly? Your doctor may ask some of the following questions. Is the pain worse in certain pairs of shoes? Does any type of activity ease the pain or worsen it? Are you having pain in any other part of your body? Non Surgical Treatment Simple treatments may be all that are needed for some people with a Morton's neuroma. They include the following. Footwear adjustments including avoidance of high-heeled and narrow shoes and having special orthotic pads and devices fitted into your shoes. Calf-stretching exercises may also be taught to help relieve the pressure on your foot. Steroid or local anaesthetic injections (or a combination of both) into the affected area of the foot may be needed if the simple footwear changes do not fully relieve symptoms. However, the footwear modification measures should still be continued. Sclerosant injections involve the injection of alcohol and local anaesthetic into the affected nerve under the guidance of an ultrasound scan. Some studies have shown this to be as effective as surgery.  Surgical Treatment If symptoms do not respond to any of the above measures then surgery may be suggested. This involves a short 30 minute operation to either remove tissue to take pressure off the nerve or to remove the nerve causing the pain. The surgery can be done as a day case but it will be two or three weeks before you can be fully active on your feet. There may be some lingering numbness afterwards if the nerve is removed. But surgery is successful in around 80% of cases. There is a small risk of complications such as infection and thickening of the skin on the soles of the feet. There are actually two different types of leg length discrepancies, congenital and acquired. Congenital implies you are born with it. One leg is anatomically shorter compared to the other. Through developmental phases of aging, the brain picks up on the stride pattern and recognizes some variation. Your body typically adapts by dipping one shoulder over to the "short" side. A difference of less than a quarter inch is not blatantly uncommon, doesn't need Shoe Lifts to compensate and ordinarily doesn't have a serious effect over a lifetime.
 Leg length inequality goes largely undiscovered on a daily basis, however this issue is simply remedied, and can eliminate many incidents of lumbar pain. Treatment for leg length inequality typically consists of Shoe Lifts. These are generally cost-effective, often being under twenty dollars, in comparison to a custom orthotic of $200 and up. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position. Chronic back pain is easily the most widespread health problem affecting men and women today. Over 80 million men and women are afflicted by back pain at some point in their life. It's a problem which costs employers millions year after year as a result of time lost and output. Fresh and better treatment methods are continually sought after in the hope of reducing the economical impact this issue causes.  People from all corners of the earth experience foot ache as a result of leg length discrepancy. In a lot of these cases Shoe Lifts are usually of worthwhile. The lifts are capable of relieving any pain and discomfort in the feet. Shoe Lifts are recommended by countless skilled orthopaedic practitioners". To be able to support the body in a well-balanced fashion, the feet have a very important function to play. Inspite of that, it is sometimes the most neglected region of the body. Some people have flat-feet which means there is unequal force exerted on the feet. This will cause other parts of the body including knees, ankles and backs to be impacted too. Shoe Lifts ensure that suitable posture and balance are restored.  Overview There are approximately 75 different causes of heel pain. At least 80% of all heel pain is due to heel spurs. A heel spur contains calcium, but cannot truly be called a calcium deposit. Bone spurs, whether they are on the heel or on any other bone of the body, are true bone -- they are true enlargements of the bone and may be sharp and pointed, or round and knobby. Since bone spurs are true bone, they contain calcium just like regular bones, but are not pure calcium deposits. Causes There exists a membrane that covers most of the bone along the heel. When this membrane gets torn repeatedly due to straining of the muscles in the foot, the calcium deposits that lead to heel spurs are more likely to occur.  Symptoms The Heel Spur itself is not thought to be painful. Patients who experience pain with Plantar Fasciitis are suffering from inflammation and irritation of the plantar fascia. This the primary cause of pain and not the Heel Spur. Heel Spurs form in some patients who have plantar fasciitis, and tend to occur in patients who have had the problem for a prolonged period of time. While about 70 % of patients with plantar fasciitis have a heel spur, X-rays also show about 50 % of patients with no symptoms of plantar fasciitis also have a heel spur. Diagnosis Diagnosis of a heel spur can be done with an x-ray, which will be able to reveal the bony spur. Normally, it occurs where the plantar fascia connects to the heel bone. When the plantar fascia ligament is pulled excessively it begins to pull away from the heel bone. When this excessive pulling occurs, it causes the body to respond by depositing calcium in the injured area, resulting in the formation of the bone spur. The Plantar fascia ligament is a fibrous band of connective tissue running between the heel bone and the ball of the foot. This structure maintains the arch of the foot and distributes weight along the foot as we walk. However, due to the stress that this ligament must endure, it can easily become damaged which commonly occurs along with heel spurs. Non Surgical Treatment In case of heel spurs rest is most important. Active sports, running, long walks etc should be avoided to start with. If you?re in a job that requires a lot of standing, take a few days off work. Rest (or reduced activity) is essential to allow the inflammation from becoming aggrevated. Furthermore, you can use ice packs (placed on the heel for 5-10 minutes) to ?cool down? the inflamed area. You may take anti-inflammatory medication or apply a topical inflammatory (i.e. a cream) to help reduce inflammation. In addition, there are some simple exercises that should be done daily to help relieve heel spur pain. Surgical Treatment In a small number of cases (usually less than 5 percent), patients may not experience relief after trying the recommendations listed above. It is important that conservative treatments (such as those listed above) be performed for AT LEAST a year before considering surgery. Time is important in curing the pain from heel spurs, and insufficient treatment before surgery may subject you to potential complications from the procedure. If these treatments fail, your doctor may consider an operation to loosen the plantar fascia, called a plantar fascia release. Overview
Bursitis is the inflammation of a bursa within the body. A bursa is a fluid-filled sac that cushions some of the major joints, allowing bones, gliding muscles, and tissues to exist together without harming each other. It aids in reducing the friction between bones and the soft tissues above it. Though there are bursae all over the body, the main ones are located in the knee, elbow, shoulder, hip, and heel. These are also the ones that are the most often injured. Still, however, when you hear the word ?bursitis?, the person is usually referring to their shoulder, but it could also refer to any of the preceding areas--such as the second most common one, the hip. Causes High impact activity, such as running. Trauma to the heel such as jumping from a height. Increase in training levels. Lack of shock absorbency in the trainers worn. Worn running shoes. Poor biomechanics. Loss of the fat pad under the heel. Increase in weight. Symptoms Pain or tenderness at the back of the heel around the Achilles region. Increased pain during activities with strong, repetitive calf contractions, walking (uphill), stair climbing, running, jumping. Pain may be worse with rest after activity (that night or the next morning) or at the beginning of the excercise. Pain when wearing shoes and the heel is getting rubbed. Bump forming on the back of the heel. Limping. Stiffness. Decreased range of motion. Redness and warmth (if the bursa gets infected). Diagnosis After you have described your foot symptoms, your doctor will want to know more details about your pain, your medical history and lifestyle, including whether your pain is worse at specific times of the day or after specific activities. Any recent injury to the area. Your medical and orthopedic history, especially any history of diabetes, arthritis or injury to your foot or leg. Your age and occupation. Your recreational activities, including sports and exercise programs. The type of shoes you usually wear, how well they fit, and how frequently you buy a new pair. Non Surgical Treatment In addition to R.I.C.E., there are a number of other treatments to reduce swelling and any associated pain or discomfort due to heel bursitis. Orthotics or change of footwear. Wearing an orthotic device such as a heel insert can encourage better mechanics in the foot and reduce irritation of the retrocalcaneal bursa. Some people do not need special orthotics but simply need to stop wearing shoes with rigid heel and ankle construction and instead wear more supportive, comfortable shoes. Shoes with an "Achilles notch," a groove in the collar at the back of the shoe to protect the Achilles tendon, can be particularly helpful. (Almost all running shoes are designed with an Achilles notch.) Stretching and physical therapy. Stretching the Achilles tendon often helps alleviate pain. Once the pain is resolved it is important for the patient to continue a regular stretching program. Regular stretching reduces the chance of recurrence. Surgical Treatment Surgery is rarely need to treat most of these conditions. A patient with a soft tissue rheumatic syndrome may need surgery, however, if problems persist and other treatment methods do not help symptoms. Prevention You may be able to prevent bursitis from happening or coming back. Continue your home treatment with rest, ice, pain relievers, and gentle exercises. When you are ready to try the activity that caused the pain, start slowly and do it for short periods or at a slower speed. Warm up before and stretch after the activity. Increase your activity slowly, and stop if it hurts. Use ice afterward to prevent pain and swelling. Change the way you do activities with repeated movements that may strain your muscles or joints. For example if using a certain tool has caused bursitis, start switching hands or change the grip size of your tool. If sitting for long periods has caused bursitis, get up and walk around every hour. If a certain sport is causing bursitis, consider taking lessons to learn proper techniques. Have an expert check your equipment to make sure it's well suited to your size, strength, and ability. If certain activities at work may be causing bursitis, talk to your human resources department about other ways of doing your job, equipment changes, or other job assignments. Protect your joints from pressure. Cushion knees or elbows on hard surfaces, and wear shoes that fit you well and have good support.  Overview OverviewThe term Hammer toe describes three unique contracture deformities of the toes. The deformities differ by the location of contracture in each joint of the toe. The three deformities include hammer toe, claw toe and mallet toe. Hammer toes may be flexible or rigid. Hammer toes are most common on the lesser toes (2-5) and may affect one or more toes simultaneously. Hallux malleus is the term used to described a hammer toe of the great toe. Hallux malleus is often found as an isolated foot problem. Hammer toes are found equally in men and women. The onset of hammer toes is between the ages of 30 and 80 years of age. Causes Hammer toes result from a muscle imbalance which causes the ligaments and tendons to become unnaturally tight. This results in the joint curling downward. Arthritis can also lead to many different forefoot deformities, including hammer toes. 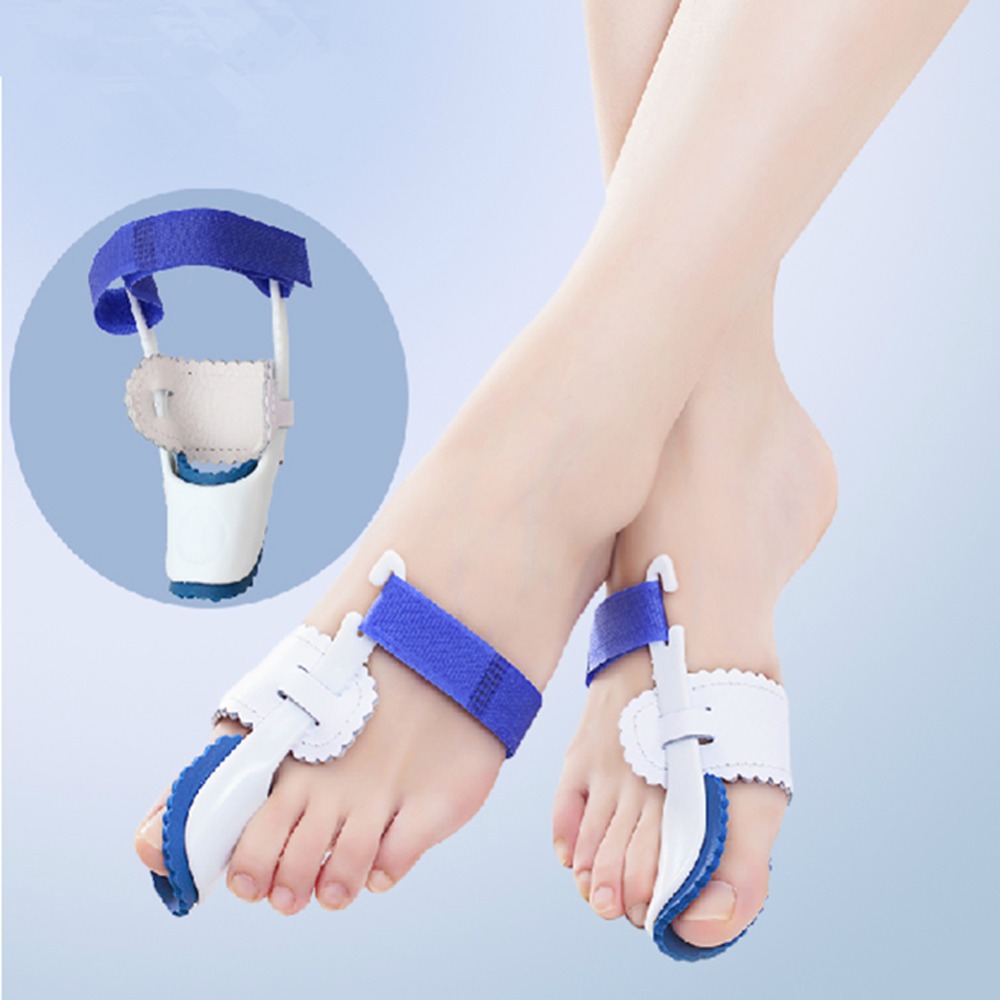 Symptoms SymptomsIf you have any of these symptoms, do not assume it is due to hammer toe. Talk to your doctor about symptoms such as a toe that curls down, corns on the top of a toe, calluses on the sole of the foot or bottom of the toe, pain in the middle joint of a toe, discomfort on the top of a toe, difficulty finding any shoes that fit comfortably, cramping in a toe, and sometimes also the foot and leg, difficult or painful motion of a toe joint, pain in the ball of the foot or at the base of a toe. Diagnosis Your healthcare provider will examine your foot, checking for redness, swelling, corns, and calluses. Your provider will also measure the flexibility of your toes and test how much feeling you have in your toes. You may have blood tests to check for arthritis, diabetes, and infection. Non Surgical Treatment If your hammertoe problem is diagnosed as flexible hammertoe, there are a number of nonsurgical treatments that may be able to straighten out your toe or toes and return them to their proper alignment. Padding and Taping. Your physician may pad the boney top-part of your hammertoe as a means of relieving pain, and may tape your toes as a way to change their position, correct the muscle imbalance and relieve the pressure that led to the hammertoe's development. Medication. Anti-inflammatory drugs such as Hammer toes aspirin and ibuprofen can help deal with inflammation, swelling and pain caused by your hammertoe. Cortisone injections may be prescribed for the same purpose. If your hammertoe is a consequence of arthritis, your physician may prescribe medications for that. Surgical Treatment For the surgical correction of a rigid hammertoe, the surgical procedure consists of removing the damaged skin where the corn is located. Then a small section of bone is removed at the level of the rigid joint. The sutures remain in place for approximately ten days. During this period of time it is important to keep the area dry. Most surgeons prefer to leave the bandage in place until the patient's follow-up visit, so there is no need for the patient to change the bandages at home. The patient is returned to a stiff-soled walking shoe in about two weeks. It is important to try and stay off the foot as much as possible during this time. Excessive swelling of the toe is the most common patient complaint. In severe cases of hammertoe deformity a pin may be required to hold the toe in place and the surgeon may elect to fuse the bones in the toe. This requires several weeks of recovery.  Prevention PreventionThe best treatment is good prevention! Hammertoe can be prevented by wearing shoes with ample toe room, avoiding high heels, and wearing adjustable shoes to assure a looser fit. When buying shoes, shop at the end of the day when your feet are swollen from daily activity, try both shoes on to confirm they fit properly, and if necessary, visit a shoe repair store to see if they can stretch your shoes for a better fit.
Overview
 In constrictive shoes, the big toe is forced to bend toward the second toe and the first joint of the big toe is moved out of place. To compensate for the realignment, the outside of the joint is increased in size. Tendons then begin to pull the toe into an abnormal position. Over time the change in position becomes painful and permanent. The change in position also causes the mechanics of the toes and foot to be affected. The joint at the base of the big toe carries a lot of weight when walking or running. In a normally shaped foot the position of the big toe helps create a wide base of support and stability. A foot that has had the big toe bent toward the second toe will tend to roll inward. This abnormal pronation, along with the ill-fitting shoes will make the Bunion even worse. If a person has a foot anatomy that is prone to Bunions, wearing footwear with a too-narrow toe box will accelerate the development of a Bunion. Wearing footwear with a wide toe box may help prevent or at least delay the development of Bunions. In constrictive shoes, the big toe is forced to bend toward the second toe and the first joint of the big toe is moved out of place. To compensate for the realignment, the outside of the joint is increased in size. Tendons then begin to pull the toe into an abnormal position. Over time the change in position becomes painful and permanent. The change in position also causes the mechanics of the toes and foot to be affected. The joint at the base of the big toe carries a lot of weight when walking or running. In a normally shaped foot the position of the big toe helps create a wide base of support and stability. A foot that has had the big toe bent toward the second toe will tend to roll inward. This abnormal pronation, along with the ill-fitting shoes will make the Bunion even worse. If a person has a foot anatomy that is prone to Bunions, wearing footwear with a too-narrow toe box will accelerate the development of a Bunion. Wearing footwear with a wide toe box may help prevent or at least delay the development of Bunions.Causes Women are particularly at risk for bunions, as high heels may help aggravate the condition. Bunions may also be caused when bursal sacs, sacs that absorb friction and lubricate the many tendons, bones muscles of the body, in the foot become inflamed or swollen. Bunions may also be prompted by the metatarsal bone, the bone that runs from the heel to the toe of the foot, with one metatarsal bone leading to each toe, of the big toe enlarging or deviating slightly to the outside of the foot. Symptoms The symptoms of a bunion include the following development of a firm bump on the outside edge of the foot, at the base of the big toe, redness, swelling, or pain at or near the MTP joint, corns or other irritations caused by the overlap of the first and second toes, restricted or painful motion of the big toe. Diagnosis Your doctor will be able to diagnose a bunion by asking about your symptoms and examining your feet. You may also have blood tests to rule out any other medical conditions, such as rheumatoid arthritis or gout, although this is rare. Your doctor may refer you to a podiatrist or chiropodist (healthcare professionals who specialise in conditions that affect the feet). Non Surgical Treatment Long-term treatment of bunions must be directed towards re-balancing the foot, so that we no longer walk with our weight forced on to the inner border of the foot. This is accomplished by controlling and reducing pronation with the use of a high quality arch support or custom made orthotics. These devices comfortably re-balance the feet and overcome pronation. This reduces the abnormal weight forces on the big toe and its metatarsal head, allowing the feet to function normally. As a result, the deformity should not worsen, and the pain should gradually subside. If the foot is not re-balanced, the deformity and pain will become worse.  Surgical Treatment Bunion surgery is most often a day case or one night in hospital. Surgery can be done under ankle block (patient awake) or general anaesthetic. It is best to rest with the foot elevated for the first 2 weeks after surgery. The foot is bandaged and a special sandal supplied by the hospital is worn for 6 weeks. Sensible shoes are to be worn for a further 6 weeks after the bandages are removed. It will take between 3-6 months for the swelling to go down. It will take 12 months before everything completely settles. It is also important to remember that not all bunion operations are entirely successful. |
|
